Blog & News
NHIS: Coverage and Uninsurance Rates Mostly Stable in January-September 2016
May 17, 2017:The National Center for Health Statistics (NCHS) released health insurance coverage estimates for January through September 20161 from the National Health Interview Survey (NHIS) as part of the NHIS Early Release Program.
In the Nation
With only a few exceptions coverage and uninsurance rates remained stable between the first three quarters of 2015 and the first three quarters of 2016.
Coverage by Type
Adults (18-64 years)
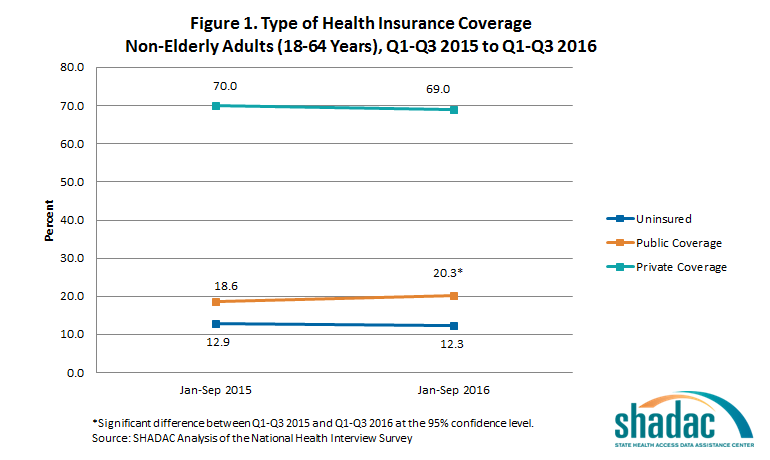
The new estimates show that among adults aged 18 to 64, only the rate of public coverage changed significantly, increasing 1.7 percentage points. Uninsurance and private coverage were statistically stable. Among this group, in the first three quarters of 2016:
- 12.3% were uninsured at the time of interview
- 20.3% had public coverage (vs. 18.6% in January-September 2015)
- 69.0% had private coverage
Children (0-17 years)
The rates of coverage for children (0-17 years) by type of coverage were statistically unchanged from the first three quarters of 2015. Among this group in January through September of 2016:
- 5.0% were uninsured at the time of interview
- 43.4% had public coverage
- 53.5% had private coverage
The Uninsured
Adults (18-64 years)
Not only did uninsurance hold steady from the first three quarters of 2015 and the first three quarters of 2016 among non-elderly adults taken as a whole, but the distribution of uninsurance among subgroups remained stable:
- Adults aged 25 to 34 years continued to be the most likely to be uninsured, with nearly twice the uninsured rate of 45-64 year olds (16.4% vs. 8.6%).
- Adults aged 18 to 24 and adults aged 35 to 44 once again had similar rates of uninsurance, at 13.6 and 14.7, respectively.
Children (0-17 years)
Uninsurace among children was stable overall between January through September 2015 and January through September 2016; however, a breakdown by poverty status and coverage type shows that the percentage of poor children (<100% FPL) with private health insurance coverage decreased significantly, from 9.6 to 7.1 percent.
Race/Ethnicity
The only racial/ethnic group that saw a statistically significant change from January through September 2015 to January through September 2016 was Hispanics/Latinos, among whom uninsurance dropped 2.1 percentage points (from 21% to 18.9%).
Enrollment in High-Deductible Health Plans
Among persons under the age 65 with private health insurance, the percentage who were enrolled in a high deductible health plan (HDHP) increased in 2016. Among this age group:
- 39.1 percent were enrolled in an HDHP (vs. 36.2% in January-September 2015)
- 15.2 percent were enrolled in HDHPs that incorporated health savings accounts (vs. 13.2% in January-September 2015)
In the States
NHIS estimates of the uninsured are available for 38 individual states with sufficient sample size for the first three quarters of the 2016 calendar year. Among states with estimates available for the first three quarters of both 2015 and 2016, the only one that saw a significant change in uninsurance was California, with a decrease of 4.5 percentage points.
State Medicaid Expansion Status
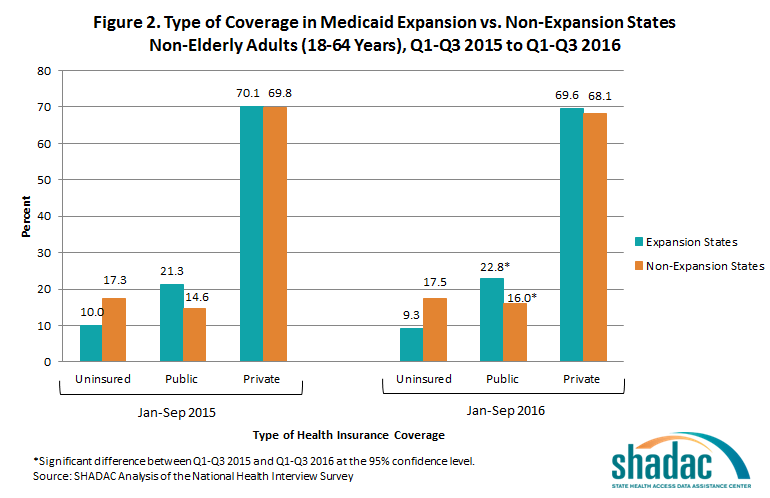
In both Medicaid expansion states and non-expansion states, rates of public coverage increased significantly among non-elderly adults (18 to 64) from the first three quarters of 2015 to the first three quarters 2016. Uninsurance rates and rates of private coverage held stable in both expansion and non-expansion states.
Among adults ages 18 to 64 living in expansion states:
- 9.3 percent were uninsured at the time of interview
- 69.6 percent had private coverage
- 22.8 percent had public coverage (up from 21.3 % in the first three quarters of 2015)
Among adults ages 18 to 64 living in states that did not expand Medicaid:
- 17.5 percent were uninsured at the time of interview
- 68.1 percent had private coverage
- 16.0 percent had public coverage (up from 14.6% in January through September 2015)
Non-elderly adults in expansion states continued to be less likely to be uninsured than non-elderly adults in non-expansion states in the first three quarters of 2016, with uninsurance in expansion states at 9.3% and uninsurance in non-expansion states at 17.5%.
View the NCHS Early Release Report, "Health Insurance Coverage: Early Release of Esimates from the National Health Interview Survey, January-September 2016."
About the NHIS Early Release Program
The new NHIS estimates were published as part of the NHIS Early Release Program, through which analytic reports and preliminary microdata files are made available on an expedited schedule so that data users have access to the most recent NHIS information without having to wait for the final annual NHIS microdata files to be released after the end of each data collection year. The early release reports and files are produced prior to final data editing and weighting.
1SHADAC's analysis differes slightly from the NCHS report because SHADAC'compares estimates from the first three quarters of 2015 with estimates from the first three quarters of 2016, while the NCHS compares the estimates for all of 2015 with estimates from the first three quarters of 2016.
Blog & News
How Would an ACA Repeal Affect Minnesota?
May 11, 2017:A new SHADAC brief examines the implications of an Affordable Care Act repeal for Minnesota. The authors, SHADAC Research Assistant Robert Hest and SHADAC Director Lynn Blewett, present an overview of the the impact of the ACA's coverage expansions in the state and highlight the potential for losses with a repeal. They look specifically at rates of health insurance coverage, hospital uncompensated care, and levels of federal health funding for Minnesota's public coverage programs.
 The authors point out that between 2013 and 2015
The authors point out that between 2013 and 2015
- The ACA reduced the number of uninsured in Minnesota by nearly 200,000 (almost one half), bringing the state's uninsurance rate down to 4.5 percent from 8.3 percent. 1
- Minnesota's hospital uncompensated care fell by $53 million (a 16.7 percent decrease). 2
With an ACA repeal
- The number of uninsured Minnesotans would more than double. 3
- Minnesota's hospital uncompensated care would increase by an estimated $548 million by 2019. 4
The authors also emphasize that individuals enrolled in health plans through MNsure received an estimated $115 million in tax credits and cost-sharing reductions from the federal government in 2016--funds that would no longer be available with an ACA repeal. 5 Moreover, the State of Minnesota stands to lose the $2 billion in annual federal funding that it currently receives for Medical Assistance and MinnesotaCare, along with $80.8 million in federal Preventional and Public Health fund grants. 6, 7
1 SHADAC Analysis of the 2013-2015 American Community Survey
2 Minnesota Department of Health: Health Economics Program. "Uncompensated Care at Minnesota Hospitals Drops for the Second Year in a Row," October 31, 2016. http://www.health.state.mn.us/news/pressrel/2016/costs103116.pdf
3 SHADAC Analysis of the 2015 American Community Survey
4 Buettgens, M., Blumber, L., & Holahan, J. "The Impact on Health Care PRoviders of Partial ACA Repeal through Reconciliation," Urban Institute, January 2017. http://www.rwjf.org/content/dam/farm/reports/issue_briefs/2017/rwjf433621
5 Kaiser Family Foundation. "Estimated Total PRemium Tax Credits Received by Marketplace Enrollees," March 31, 2016. http://kff.org/health-reform/state-indicator/average-monthly-advance-premium-tax-credit-aptc/
6 Minnesota Department of Human Services. "Repealing the Affordable Care Act: Impacts to Minnesota's Public Healthcare Programs," January 6, 2017. http://mn.gov/dhs/aca-repeal/issue-brief/
7 Trust for America's Health. "Minnesota Could Lose More than $80 Million to Fight Health Epidemics over Five Years if the ACA and Prevention and Public Health Fund Are Repealed," 2017. http://healthyamericans.org/reports/prevention-fund-state-facts-2017/release.php?stateid=MN
Publication
Impact of the Affordable Care Act in Minnesota: Implications of Repeal
In this brief, the authors present an overview of the impact of the ACA’s coverage expansions in the state of Minnesota and highlight the potential for losses with an ACA repeal. We look specifically at rates of health insurance coverage, hospital uncompensated care, and levels of federal health funding for Minnesota's public coverage programs.
Publication
SHADAC Newsletter - January 2017
The SHADAC newsletter contains updates on SHADAC activities, news from the states, resource updates, and blog highlights. Subscribe to our newsletter here.
Blog & News
State Medicaid Access Review Monitoring Plans (ARMPs): An Early Look at Data Sources Used by States
December 13, 2016:In November 2015, the Centers for Medicare and Medicaid Services (CMS) issued a final rule implementing Medicaid’s “equal access” provision, nearly 25 years after the statute was enacted and more than four years after the rule was initially proposed. One piece of the final rule requires that states develop Access Review Monitoring Plans (ARMPs) to address and analyze the extent to which the health care needs of Medicaid fee-for-service (FFS) beneficiaries are met, the availability of health care and providers, changes to beneficiary utilization, as well as comparisons of payment rates.
ARMP Requirements
CMS grants states significant flexibility in selecting measures and defining their approach to the plans. However, states are required to analyze certain services (described below) and incorporate beneficiary and provider input on ARMPs. Final baseline reports were due to CMS on October 1, 2016; states are required to submit a revised plan every three years or in the event of a FFS rate reduction or a high volume of complaints about access to a service in a particular geographic area.
Limitations of ARMPs
ARMPs are meant to support CMS’s goal of assuring access to covered services in FFS Medicaid, but they are not without limitations. Notably, the plans only cover access and payment rates for FFS beneficiaries, and states have increasingly turned to managed care for delivery of care to Medicaid beneficiaries. States may also struggle with the availability of timely data and the challenge of conducting data analysis and producing triennial plans without federal funding. Despite these limitations, baseline ARMPs may shed light on states’ access priorities and approaches to analysis.
Examining ARMP Data Sources: Our Approach
In an effort to identify the range of data states leveraged in ARMPs, SHADAC researchers performed a key word search online and on State Medicaid and Dept. of Health websites during the month of November 2016 (one month after final reports were due) to identify draft or, if available, final ARMPs. We then abstracted key information about data sources and service categories to a table. We identified a total of 43 ARMPs, of which 19 were final. The summary below is based on all plans, including draft plans but relying on final plans when available.
Service Categories
All states are required to cover access to primary care, including dental services, specialty, behavioral health, obstetrics and gynecology (including labor and delivery), and home health services. These services were included for analysis in all plans identified. However, although the final rule included dental services in its definition of primary care, only 29 of the 43 states included these services in ARMPs. One state explicitly excluded dental services from analysis based on their interpretation of the final rule’s requirements for analysis of primary care. Some ARMPs examined services beyond those required in the final rule such as durable medical equipment (AZ), transportation (IN), and nursing facility services (PA).
Results: Data Sources Used
Nearly every state analyzed access using Medicaid Management Information Systems (MMIS) data (i.e., provider, individual enrollment and/or claims data), which states are required to use for mechanized claims processing and information retrieval. Approximately fifteen also included FFS Consumer Assessment of Healthcare Providers and Systems (CAHPS) data in their analyses, and many states said they would try to leverage data from the national CAHPS survey in future analyses where state level FFS CAHPS data wasn’t currently available. Eight states included (or would include in future plans) beneficiary reported access issues from call center data. Some states explored additional data sources including Census data (CA, CT, NV, ME), state-specific surveys (e.g., CO Health Access Surveys and MN Health Care Access Survey), and Healthcare Effectiveness Data and Information Set (HEDIS) measures (OH, MA, MN, SC, CT).
Potential Limitations to Reliance on MMIS Data
As mentioned above, states rely heavily on MMIS data for access analyses. Though this may reduce the administrative burden of data collection, MMIS data may not provide a complete picture of access. There are well-documented limitations to using MMIS data for patient identification as well as uncertain validity of encounter data and completeness of diagnosis information. Moreover these data were not intended for use in research. States will likely need to supplement MMIS data with other data sources to ensure an accurate reflection of access in their ARMPs.
Looking Ahead: How CMS Can Support State Efforts to Measures Access
Initial state plans are currently under CMS review. Plans are expected to change over time resulting from this review and as priorities, delivery systems, and data availability shift over time. Going forward, CMS can support states by identifying and disseminating promising data sources and approaches to measuring access, especially those not commonly used by states, and sharing solutions to common barriers to access data collection and analysis.